Lab and diagnostic tests for pregnancy
Lab tests
The most complete battery of lab tests are performed during the first trimester. Blood type will be requested and if the woman is Rh negative the type and Rh of the father of the baby will also be requested in order to determine if a possible Rh incompatibility exists (a possible blood incompatibility will only exits if the mother is Rh negative and the father is Rh positive). In this situation an anti-Rh vaccine is given intramuscularly to the mother in the 28th week of pregnancy. In some cases this vaccine has already been administered for other reasons during pregnancy, for example, before an invasive test like as amniocentesis, and repeating the dose at 28 weeks is unnecessary.
A serology test will also be requested during the first trimester. This blood test identifies antibodies in the serum for diseases such as rubella, hepatitis, HIV, toxoplasmosis, etc.
Toxoplasmosis is a common infection caused by the parasite Toxoplasma gondii and can be dangerous to unborn children. The most common way of contracting the parasitic infection is through exposure to cat faeces, or by eating raw or undercooked meat that contains the parasite. Other sources of infection include raw goat’s milk, raw eggs and insects such as flies and cockroaches that may have been in contact with cat faeces. Cats often become infected by eating an infected bird or a rodent. The parasite reproduces in the cat’s intestines and is expelled in its faeces. Toxoplasmosis is uncommon in pregnant women and does not pose a major threat and subsequent checks are performed during pregnancy. Most often, as we have explained, it is included in the first trimester serology test (the immunity test). Thus pregnant women will know if they have had the disease and if they are immune to possible contagion, or, on the other hand, if they have never contracted the disease and therefore are susceptible to infection.
Pregnant women not immune to toxoplasmosis are advised to:
- Do not handle cat faeces or the kitty litter they use. If you have garden or planters wear gloves when working with soil.
- Do not eat raw or undercooked meats, especially lamb and pork. Meat should be cooked at high temperatures. Immediately wash hands with soap after handling raw meat.
- Do not touch your nose, mouth or eyes with potentially infected hands.
- Do not eat raw meat; meat must be cooked or fried.
- Wash both fruits and vegetables.
Second trimester lab tests are similar to the first trimester, and while less extensive they include a special test, called the O’Sullivan test.
The O’Sullivan test is a sugar tolerance during pregnancy test. Some patients may develop a type of diabetes during pregnancy called gestational diabetes, which is diagnosed by administering sugar and analysing if it is removed properly. In this test 50 gr of glucose is administered on an empty stomach and blood glucose is measured an hour later. If blood glucose is higher than 140 mg/dl, an additional test will be required to determine whether gestational diabetes is the cause, as in some cases sugar can be improperly metabolised in the short term while actually being normal in the long term.
The glucose tolerance test is accomplished by administering 100 g sugar orally and taking a blood sample to measure blood sugar at 60, 120 and 180 minutes. Should two readings be out of range the patient will be sent to the endocrinology unit, which will manage the pregnancy together with the gynaecologists to avoid any complications. Today, and with all the advances in both diagnosis and treatment, women should not worry about developing diabetes during pregnancy and in virtually all cases blood sugar levels normalise post pregnancy.
A number of tests are performed during the third trimester, including coagulation tests, which are required by the anaesthetic unit to verify that there is no contraindications to an epidural during childbirth.
A screening test called a triple screen is often performed between the 12th and 16th week in addition to these three coagulation tests, as appropriate, to rule out foetal chromosomal abnormality. This test, taking into consideration the mother’s background, the 12-week ultrasound and a series of blood test results, determines each patient’s statistical probability of having a child with a chromosomal abnormality. It is not a 100% certain diagnosis and is merely indicative. This test is not required for patients whose background or age puts them at risk for amniocentesis or other invasive prenatal diagnosis techniques. Likewise, when the triple screen results in high probability (more than 1/270), genetic testing using an alternative test is recommended.
Another analysis conducted during weeks 32-34 is the vaginal and rectal swabs to diagnosis infection by a bacterium called Streptococcus agalactiae beta. This test is painless and simple involves removing a sample of vaginal fluid with a cotton pad. A study carried out a few years ago found that very few children were infected at birth, but those that were might have become infected because the mother was a carrier of bacteria called streptococcus in the vaginal mucosa.
Why some mothers are carriers and others are not is unknown, and so all expectant mothers are tested and those that have the bacteria in the vaginal or rectal floral are given an antibiotic during delivery to prevent possible neonatal infection.

Diagnostic tests
A pelvic ultrasound is a diagnostic method that uses high-frequency sound waves. Obstetrician gynaecologists use this test to determine if a woman is pregnant and assess the condition of the embryo or foetus. No harm is caused to the mother or the foetus because ionizing radiation is not used. While there is a general guideline for ultrasound, which will be discussed below, individualised ultrasounds might be necessary in specific cases.
- Establish the existence of an intrauterine pregnancy.
- Determine if it is a single or multiple pregnancy.
- Estimate how far along the pregnancy is.
- Diagnose birth defects.
- Determine the position of the foetus and its estimated weight.
- Examine the position of the placenta and the amount of amniotic fluid.
Ultrasounds are usually performed vaginally during the first trimester (until week 13-14), since a higher resolution image is obtained. However, an abdominal ultrasound is usually performed after 14 weeks, except in specific cases where certain parameters such as cervical length or the position of the placenta needs to be determined.
The number and timeline of ultrasounds during pregnancy depends on each particular case.
If possible, four ultrasounds are regularly recommended:
- Confirmation of pregnancy (6-8 weeks)
- First trimester (11+6/13+6 weeks)
- Second trimester (20-22 weeks)
- Third trimester (28-37 weeks)
Obstetric ultrasound by trimesters
Although an initial ultrasound is sometimes performed around week seven or eight of pregnancy, it is standard to establish the first fundamental ultrasound at 12 weeks.
It is performed abdominally or transvaginally according to the method that will produce the best image. It is recommended that the patient eat before the test.
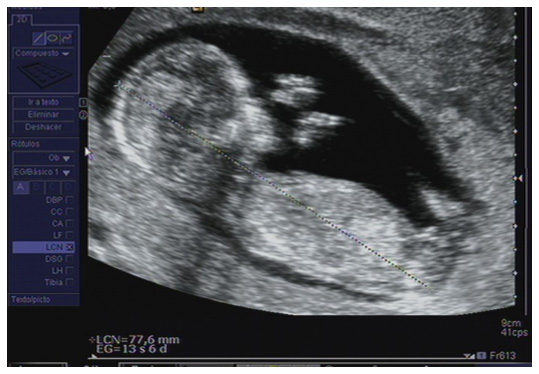
- Date the pregnancy (embryo size by crown-rump length) and set the number of foetuses (single or multiple gestation).
- Pregnancy viability (heartbeat).
- Evaluate the presence of ultrasound markers for the Down Syndrome risk index and other chromosomal abnormalities (nuchal translucency or fold, ductus venosus, nasal bones and tricuspid regurgitation, etc.).
- Eliminate the presence of foetal malformations at an early stage.
It is performed between weeks 20 and 22 of pregnancy. In special cases it will be performed at week 19. This ultrasound is considered the most important because the baby is fully formed at this point and all internal organs, especially the proper functioning and development of the heart, can be virtually displayed. The position of the placenta, that is, its location within the uterus and the amount of amniotic fluid, can also be determined.
It is performed abdominally. In some cases it can be performed transvaginally for a foetal morphological examination than cannot be seen well abdominally or to access the placenta position and cervical length.
- First, to define the time of amenorrhea, number of foetuses, foetal statistic, chorionicity and amnionicidad.
- Foetal biometry: biparietal diameter (BPD), head circumference (HC), abdominal circumference (AC) and femur length (FL).
- Evaluate adnexal structures: placenta, umbilical cord and amniotic fluid.
- Morphological study for screening of foetal structural malformations, performing comprehensive monitoring of the foetal anatomy (head, face, chest, heart, abdomen, genitals, spine and limbs).
- Doppler study if deemed necessary: foetal flow (umbilical artery and middle cerebral artery) and maternal flow (uterine arteries).
- Cervical length (as applicable).
- Associated breast disorders (fibroids, adnexal cysts, etc.).

It can be performed from 28 to 37 weeks, with the optimum period being from week 30 to 34.
It performed abdominally. In some cases it can also be performed transvaginally to assess the placenta and cervical length.
- Assess foetal position: the foetus is usually in the vertex position in the third trimester.
- Measurement of foetal biometry and estimated foetal weight, screen for growth disorders (foetal growth delays and foetal macrosomia).
- Detection of diseases that mainly appear in the third trimester (skeletal dysplasias, lesions of the central nervous system, obstructive renal disease, gastrointestinal disease, heart disease, late-onset arrhythmias and foetal tumour pathology)
- Study of foetal wellbeing (foetal movement, amniotic fluid volume) and measurement of foetus arterial and venous flow parameters in special cases (foetal Doppler).
- Location of the placenta and cord pathology.

Three-dimensional ultrasound (3D) is a three-dimensional representation of images obtained by conventional two-dimensional ultrasound. 4D ultrasound is a technique to see the foetus move in three dimensions and in real time. This technique makes it possible to see the foetus moving inside the womb. Images are often high quality and extremely realistic, making it possible to see how the foetus behaves in the womb, like smile, move the face and yawn. Studies show that this technique increases bonding between parents and the unborn child. However, while this ultrasound is basically performed for fun, 4D ultrasound provides relevant information concerning the degree of malformation in certain foetal conditions like a cleft lip. While 4D ultrasound can be performed at any time during pregnancy, weeks 27-32 of pregnancy is the ideal time to observe more defined and developed facial features. The technique has certain limitations and not all images have the same definition; for example, the amount of amniotic fluid, foetal position, the position of the placenta and certain maternal conditions such as obesity diminish optimal images from being taken.
There are technical advances in the field of prenatal diagnosis that make an early diagnosis of a high percentage of congenital anomalies possible.
First we must understand the difference between a chromosomal and genetic alteration. A foetal chromosomal abnormality is the lack, excess or alteration of a foetal chromosome. All our cells have 23 pairs of chromosomes. Each pair contains a chromosome from the mother’s egg and one that comes from the male sperm. Each chromosome is composed of thousands of genes. We can study the chromosomes, although it is impossible to study each gene. For example, Down syndrome is a chromosomal disorder that we can diagnose (pair 21 has three chromosomes instead of two) whilst we cannot diagnose cystic fibrosis, a genetic alteration inside the gene that available invasive tests are unable to diagnose.
Prenatal invasive diagnostic techniques makes it possible to determine the foetal karyotype (foetal chromosome or genetic map) by taking certain samples depending on the chosen technique.
Invasive technique in which a sample of chorionic villus (placenta) is taken to study the foetus karyotype (chromosome analysis). The preferable way to take the sample is vaginally.
It is usually performed between weeks 11 and 13+6 of pregnancy. Patients are recommended to have a full bladder, eat and be calm before taking the test. There is a 0.5-1% risk of complications (foetal loss, infection, amniotic sac rupture, hematoma, etc.). If the patient is Rh negative anti-D gamma globulin is administered within the 72 hours following the test. Relative rest is recommended 48 hours after the test. An ultrasound to monitor progress will be performed 7 to 10 days after the test.
This is the extraction of foetal amniotic fluid using a very thin needle through the mother’s abdomen. Foetal cells are extracted from this liquid to analyse the chromosomes. This puncture is performed using ultrasound guidance. The final results take about 3-4 weeks to be possible, although it is possible to determine whether chromosome pairs 13, 18, and 21 and the X and Y chromosomes (these are the most commonly altered) are altered within 48-72 hours if a test called PCR is performed. This test is performed between weeks 14 and 16 of pregnancy.
The risk of complications is 1% (foetal loss, infection, amniotic sac rupture, etc.).
If the patient is Rh negative anti-D gamma globulin is administered within the 72 hours following the test. Relative rest is recommended 48 hours after the test. An ultrasound to monitor progress will be performed 7 to 10 days after the test.
Invasive technique that involves puncturing the umbilical vein using a needle through the abdomen in order to extract foetal blood.
It is commonly indicated to quickly determine foetal karyotype starting at week 18 of pregnancy, analysis of foetal acid-base balance, foetal infections, intrauterine transfusion and determining the degree of foetal anaemia in cases of isoimmunisation or other genetic haematological disorders.
This test is not recommended before week 18-20 pregnancy.
There is a high risk of complication, the most common being: foetal loss (1.4-1.9%), miscarriage, structural damage to adjacent organs (bladder, intestines), wall hematoma, chorioamnionitis and bleeding umbilical cord.
This technique should be performed by experienced staff.
Starting at 38 weeks the most reliable way to analyse foetal wellbeing is by using an electronic foetal monitors, also called a cardiotocograph or “belt“. The test lasts about 15-20 minutes, during which the woman must remain lying down. A device with two transducers placed on the mother’s abdomen. One of these transducers makes it possible to hear and assess the foetal heartbeat and the other measures the tone of the uterine muscle, that is, if the mother has contractions. Foetal movement is also assessed. CTGs will be performed each week until delivery, along with pelvic exams to check if the cervix has begun to dilate and if the baby’s head is correctly positioned.
Chart of diagnostic and analytical tests performed during pregnancy.
| WEEK OF PREGNANCY | 8 | 12 | 16 | 20 | 24 | 28 | 32 | 34 | 36 | 37 | 38 | 39 | 40 |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Weight | x | x | x | x | x | x | x | x | x | x | x | x | x |
| Blood pressure | x | x | x | x | x | x | x | x | x | x | x | x | x |
| Foetal position | x | x | x | x | x | x | x | x | x | x | |||
| Type and RH | x | ||||||||||||
| Complete lab work | x | x | x | ||||||||||
| Serology | x | x | x | ||||||||||
| Triple Screen | x | ||||||||||||
| O’Sullivan +/- SOG | x | ||||||||||||
| Transvaginal ultrasound | x | x | |||||||||||
| Abdominal ultrasound | x | x | x | ||||||||||
| Amniocentesis | x | ||||||||||||
| CTG | x | x | x | ||||||||||
| Vaginal culture | x | ||||||||||||
| Anaesthesia consultation | x |
 English
English Español
Español Català
Català